MNCH+N-Strengthening Bauchi State Frontline Capacity for Quality Maternal Newborn and Child Health Services
AN EPIC SUCCESS STORY
Better Skills, Better Outcomes: Strengthening Bauchi State’s Frontline Capacity for Quality Maternal, Newborn and Child Health Services
Background
Bauchi State faces a persistent burden of high maternal and under-5 mortality rates of ≈1500 deaths per 100,000 live births1 and 153 deaths per 1000 live births, respectively, exceeding the national averages of 512 maternal deaths per 100,000 live births and 132 deaths per 1000 live births, respectively2,3.
EpiC is supporting the government of Bauchi State through its Ministry of Health and State Primary Health Care Development Board (BSPHCDB) to address gaps in maternal, newborn, child health and nutrition (MNCH+N) services by improving access to and the quality of integrated MNCH+N services across 16 priority high-burden LGAs.
To improve the quality of care and close gaps in MNCH+N services, EpiC is strengthening the healthcare system by systematically enhancing healthcare workers’ competencies across the 16 LGAs through 24 mentorship hubs established using a hub-and-spoke model. EpiC is deploying a low-dose high-frequency (LDHF) training strategy through these mentorship hubs. LDHF training is an evidence-based alternative to traditional training models that focuses on concise, targeted, and repeated on-site learning sessions, complemented by ongoing mentorship and supportive supervision.
Hence, EpiC, in collaboration with the State, conducted a 7-day Integrated Refresher Training from April 16–22, 2026. The training workshop brought together key maternal, newborn, and child health (MNCH) stakeholders from the 16 LGAs and State-level MNCH supervisors, including LGA MCH and deputy MCH focal persons, MNCH staff from the Bauchi State Primary Health Care Development Board (BSPHCB), the Bauchi State Health Management Board (HMB), EpiC consultants from the 16 supported LGAs, and Subject matter experts.
The refresher training of trainers (TOT) workshop aimed to strengthen the competencies of the cohort of mentors who would operationalize these mentorship hubs. The mentors will provide mentorship across Basic Emergency Obstetric and Newborn Care (BEmONC/ENCC), Integrated Management of Childhood Illness (IMCI), Quality of Care (QoC), and Maternal and Perinatal Child Death Surveillance and Response (MPCDSR) through the mentorship hubs. The training employed an integrated approach to reinforce the continuum of care while linking clinical skills, quality improvement, and accountability mechanisms.
Training Overview
- Duration: 7 days
- Participants: 80 participants comprising MCH LGA and State level supervisors (midwives, nurses, public health officers, CHEWs, facility managers, and EpiC consultants)
- Coverage: 16 priority LGAs
- Key Training Components:
- BEmONC/ENCC (Days 1–3)
- QoC/ MPCDSR (Day 4)
- IMCI (Days 5–6)
- Quality of Care (Day 7)
Key Learning Areas
- Improved Clinical Competence in Basic Emergency Maternal and Newborn Care (BeMONC &ENCC Services)
Participants updated their knowledge and strengthened skills in managing obstetric and neonatal emergencies, including pre‑eclampsia/eclampsia, neonatal resuscitation, essential newborn care, and postpartum haemorrhage. Didactic lecture discussions updated knowledge, while practical simulations, demonstrations, and return demonstrations reinforced learning and improved confidence and adherence to national protocols.
Pre-Eclampsia and Eclampsia: Participant skills were strengthened through didactic lecture discussions, practical hands-on demonstrations, and return demonstrations using case studies. More than half (56.5%) of the participants reported the management of Pre-Eclampsia and Eclampsia as a key learning from the training, while 93.5% reported greater confidence in their Pre-Eclampsia/Eclampsia management skills.

Pre and post-test assessments were conducted. The questions comprised 20 multiple-choice questions covering diagnostic criteria, pharmacological management (Magnesium Sulphate and antihypertensives), clinical decision-making, convulsion response, and delivery protocols.
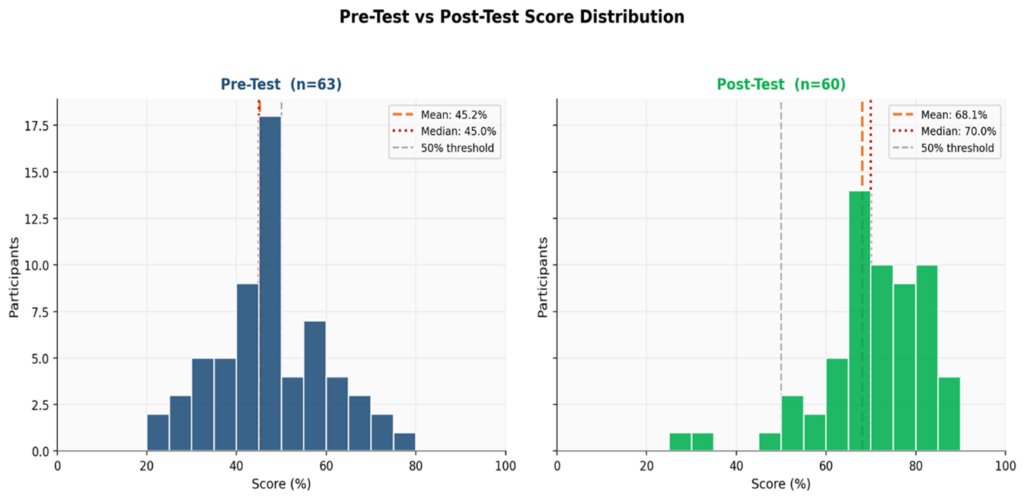
Key Finding: Pre- and post-test scores showed improvements, with mean scores rising from 45.2% to 68.1% (50.8% performance improvement). The proportion of participants who scored below 50% dropped from 66.7% to 5%, while the proportion who scored 70% or more rose from 4.8% to 55.0%.
- Labour, delivery, and essential newborn care: Participants’ learning centred on discussing scenarios around respectful maternity care, monitoring labour using the partograph, delivery of the baby, Kangaroo mother care (KMC), and essential newborn care. Hands-on skill building using simulations of case scenarios, demonstrations, and return demonstrations helped consolidate learning and build confidence.

- Pre- and post-tests consisted of a 23-multiple-choice assessment covering active labour, fetal heart rate monitoring, hand hygiene protocols, prevention of birth complications, partograph use, oxytocin administration (PPH prevention), perineal care, and essential newborn care.
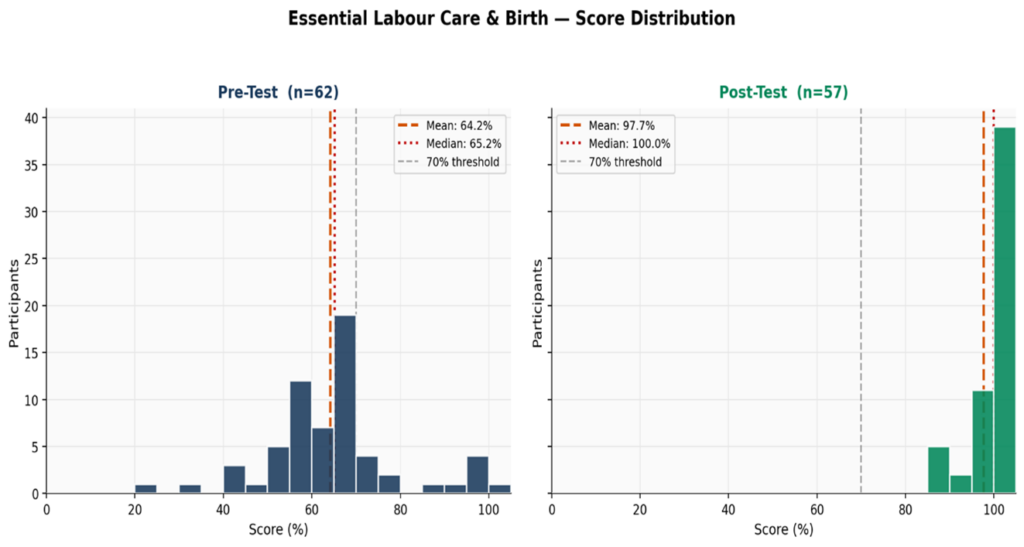
Key Finding: The training delivered a significant knowledge improvement. Participant scores improved, from a mean score of 64.2% to 97.7% (52.3% performance improvement). The proportion of participants scoring above 90% surged from 9.7% to 91.2%.
- Bleeding After Birth (Postpartum Haemorrhage [PPH]): Lecture discussions, including case scenarios, demonstrations, and return demonstrations, enhanced participants’ skills and addressed incorrect practices in the active management of the third stage of labor (AMTSL). Participants learned the correct methods for controlled cord traction and for managing PPH (blood loss ≥500 mL or 300-499 mL with one or more warning signs), retained placenta, atonic uterus, and tears.


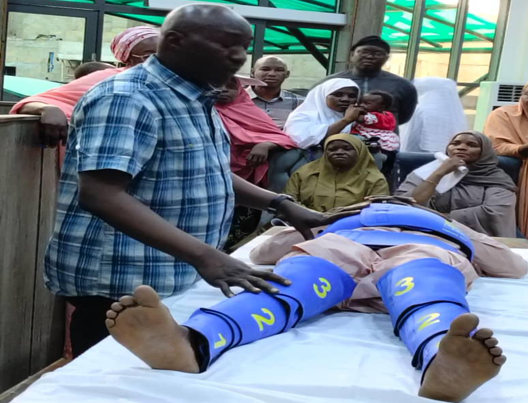
Pre and post-test comprised 15 multiple-choice questions that assessed participant knowledge of AMTSL, EMOTIVE, uterotonic medication protocols, bimanual compression, uterus tone assessment, referral criteria, and oxytocin administration.
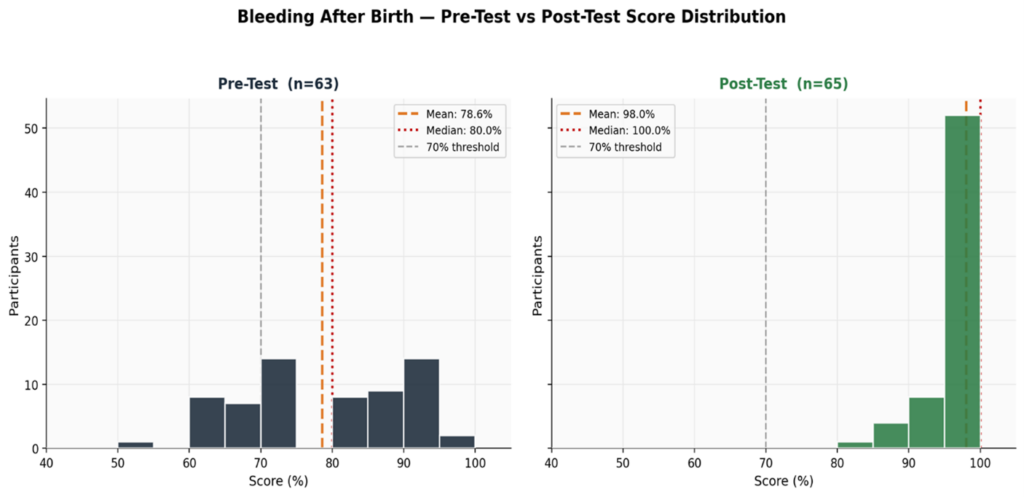
Key Finding: Training produced a remarkable improvement in knowledge. Participant mean scores increased from 78.6% to 98.0% (24.7% improvement). The proportion of participants scoring 90% and above surged from 25.4% to 92.3%.
- Strengthened Case Management for Childhood Illnesses
- Integrated Management of Childhood illnesses: This focused on strengthening the capacity of the participants in the management of the four main causes of death in children under-five (NDHS 2018)
- Malaria
- Diarrhoea
- Pneumonia
- Malnutrition (this is an underlying factor in over 50% of deaths)
Through the IMCI modules, participants enhanced their ability to assess, classify, and treat common childhood illnesses using standardized tools, reducing reliance on presumptive treatment and improving referral decision‑making. Hands-on interactive sessions using case studies helped improve learning.


The Quality-of-Care module deepened participants’ understanding of how respectful care, adherence to standards, teamwork, and QI processes directly influence maternal and child health outcomes. Participants identified facility‑specific quality gaps and discussed feasible improvement actions. Lecture discussions and practical sessions strengthened participant capacity to.
- Identify a problem in their facility, form a team, and write an aim statement
- Analyse the problem and measure the quality of care
- Develop and test changes using PDSA cycles
- Sustain improvement


Pre and post-tests comprised multiple-choice questions that assessed participants’ knowledge of conducting quality improvement activities, including developing and testing changes using PDSA cycles.
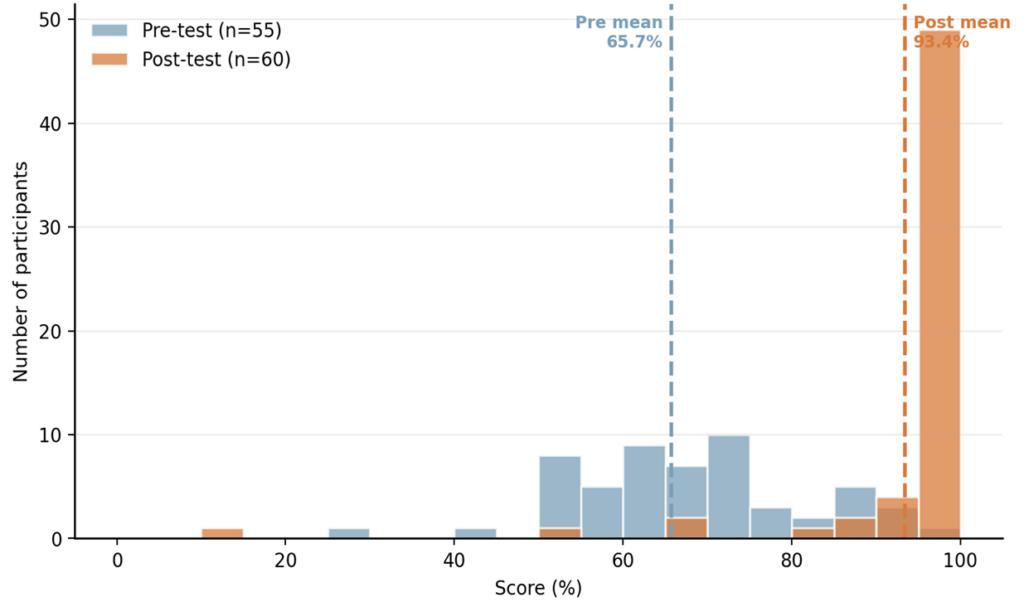
Key Finding: Training produced a significant improvement in knowledge. Participant mean scores increased from 65.7% to 93.4% (42.2% improvement). The proportion of participants scoring 90% and above surged from 9% to 90%.
- Reinforcing Accountability through MPCDSR
The MPCDSR sessions enhanced understanding of death notification, review processes, and action tracking. Participants recognized the importance of translating reviews into preventive actions rather than viewing MPCDSR as a fault‑finding exercise. Many (67%) committed to early notification of maternal and perinatal death within 24 hours and reactivating regular MPCDSR meetings aimed at preventing maternal and perinatal deaths.


Key Insights
Many participants expressed enthusiasm to operationalise the mentorship hubs and cascade the knowledge and skills gained from the TOT workshop to supervisees. More than half (71.7%) reported that they would conduct regular on-the -job coaching and mentorship, while about 20% reported integrating lessons into routine team meetings and briefings.
Human Impact Voices
During the training, I realized that using the IMCI chart booklet for assessing and classifying sick children is much simpler and more systematic than I thought. I used to rely on assumptions, but now I will carefully follow the steps, checking signs, classifying correctly, and giving appropriate treatment. This has improved my confidence and accuracy in managing children under five. -Nurse
I have been using the IMCI chart for over 3 years, but this training showed me the proper application and how to navigate the IMCI resources properly-Midwife
Given the correct dose of magnesium sulphate can save a woman’s life-CHEW
Before, I just recorded blood loss by assumption without knowing that there are measuring tools like the calibrated drape-CHO
Treatment of PPH by using EMOTIVE (PPH Care bundle), very interestingly, changed my thinking-CHEW
The story of Mrs X. made me understand that, as long as there is proper documentation, changes can be made to a recurring issue. Nothing is out of place when it comes to health investigation-EpiC MNCH Consultant
The training changed my thinking, especially on respectful maternity care, -Nurse
The training refined my approach to supportive supervision. The need to prioritize real-time case review and engagement with frontline staff to improve consistency in managing complications and strengthen accountability at the facility level. – EpiC MNCH Consultant
Lessons Learned
- Integration of clinical skills, QoC, and MPCDSR reinforced end‑to‑end service delivery, helping participants see how quality lapses contribute to preventable deaths.
- Hands‑on practice, demonstrations, and case scenario simulations were consistently identified as the most effective learning methods.
- Many participants highlighted persistent challenges related to staffing (52.2%), commodities (71.7%), and job aids (73.9%) that require system‑level support alongside the training to enable them to implement learning effectively.
- Peer learning and experience sharing surfaced locally relevant solutions that can inform future mentorship and supervision, such as strengthening respectful maternity care and leveraging social welfare schemes at the State level to overcome financial barriers to care.
Immediate Training Outcomes
- Increased confidence among participants to manage obstetric emergencies, including Pre-eclampsia/Eclampsia and PPH, manage labour and delivery, and severe childhood illnesses, document correctly, and mentor others.
- Renewed commitment by supervisors to strengthen mentorship and supervision in the PHCs and enhance quality improvement activities and MPCDSR meetings.
- Clear identification of areas requiring post‑training mentorship and supportive supervision in their LGAs and facilities.
Recommendations
- Support step-down training and refresher training to reinforce the continuum of care, sharpen skills, and improve maternal and child health outcomes.
- Strengthen post‑training follow‑up through mentorship and supportive supervision.
- Use lessons from MPCDSR to guide targeted quality improvement actions at facility and LGA levels.
Conclusion
The 7-day integrated refresher training strengthened competency, closed knowledge gaps, and standardized learning across mentors. It demonstrated that combining training in clinical skills, quality improvement, and accountability mechanisms strengthens healthcare worker capacity and reinforces linkages in the continuum of care more effectively than siloed training. Sustained follow-up through the mentorship hubs and system support will be essential to translate learning into improved maternal, newborn, and child health outcomes in Bauchi State.

References
- Ihekweazu C. Against all Odds, a small Miracle is taking place in Bauchi. Nigeria Health Watch [Internet]. 2015 Jul 7 [cited 2026 Apr 25]. Available from: https://articles.nigeriahealthwatch.com/against-all-odds-a-small-miracle-is-taking-place-in-bauchi/
- National Population Commission (NPC) [Nigeria] and ICF. 2019. Nigeria Demographic and Health Survey 2018.Abuja, Nigeria, and Rockville, Maryland, USA: NPC and ICF. NDHS 2018.pdf [Internet]. [cited 2026 Apr 25].Available from: https://www.dhsprogram.com/pubs/pdf/fr359/fr359.pdf
- 2021 MICS full report .pdf [Internet]. [cited 2026 Apr 25]. Available from: https://www.unicef.org/nigeria/media/6316/file/2021%20MICS%20full%20report%20.pdf

